Sunday, January 10, 2010
One VERY important fact....
Saturday, January 9, 2010
Pertrussis Facts:
What is Pertussis (whooping cough):
Your child can be exposed to pertussis and you may never know it, it is a hidden disease in adults and older children that becomes deadly for infants under 15 months. NO baby is safe from this and parents need to know that. It is as common and contagious as the common cold. Pertussis, more commonly known as whooping cough, is caused by a bacterium (germ), Bordetella pertussis, that lives in the mouth, nose and throat but ultimately affects the lungs. The germ is highly contagious and is easily spread from person-to-person. Pertussis, also known as whooping cough, is a potentially deadly bacterial infection that can strike at any age, but is particularly dangerous for babies. The sounds of pertussis are like no other, marked by a “whoop” made when gasping for breath after a severe coughing attack. Although in some cases the cough is the same, but the marked "whoop" may not be present.
Adults and older children can have pertussis and never know it, it does not affect them the way it affects infants. They may get it over without ever even getting treatment but they can also pass it on to a baby who cannot overcome it without treatment. Perfectly healthy babies can loose their lives to this disease in the blink of an eye.
Despite the effectiveness of vaccination, pertussis continues to occur in the United States among all age groups. Anyone who has not had pertussis previously or who has not received the pertussis vaccine can get the disease. Immunity following disease or vaccination is not lifelong. Older children, adolescents and adults can become susceptible to pertussis five-to 10-years after their last dose of pertussis-containing vaccine. Older children and adults can carry the germ and spread it even though their cold-like symptoms may be so mild they might not seek medical care.
Symptoms usually appear five-to 10-days after exposure, but can take as long as 21 days. The first symptoms are similar to those of a common cold -with cough being the most prominent. Some children will only have hte cough, fever is usually mild to none and some children, particaulary older children, may exhibit severe cold like symptoms. Runny nose, sneezing, etc. The cough gradually becomes severe and, after one to two weeks, the patient has spasmodic bursts of numerous, rapid coughs. The characteristic high-pitched "whoop," which is more common in children, comes from breathing in after a coughing episode. During such an attack, the patient may turn blue, vomit and become exhausted. Between coughing attacks, the patient usually appears normal.
Coughing attacks occur more frequently at night. The attacks increase in frequency for a couple of weeks, remain at the same level for two-to three-weeks, and then gradually decrease. Coughing may last as long as 100 days. Cough medicines usually do not help eliminate this cough. Recovery is gradual, but coughing episodes can recur for months after the onset of pertussis.
How is it spread?
Pertussis spreads easily from person to person. People get pertussis by breathing in droplets expelled from the nose or throat of an infected person during coughing or sneezing. It is also spread by direct contact with discharges from the nose or throat of an infected personComplications of Pertussis:
- Babies may bleed behind the eyes and in the brain from coughing.
- The most common complication is bacterial pneumonia. About 1 child in 10 with pertussis also gets pneumonia, and about 1 in every 50 will have convulsions.
- Brain damage occurs in 1 out of every 250 children who get pertussis.
- Pertussis is one of the top causes of infant deaths each year in the United States.
Pertussis is usually treated with a multi-day course of a mixture of appropriate antibiotics, such as azythromycin, erythromycin or clarithromycin, or an acceptable alternative. Most infants need to be hospitalized and given oxygen. People in close contact with children or adults with pertussis usually need to be treated with antibiotics and efforts should be taken to minimize an infant’s exposure to children and adults with cough illnesses.
Prevention:
Every child should get pertussis vaccine at 2, 4, 6 and 15 months of age and another dose at 4 to 6 years of age. This vaccine is given in the same shot with diphtheria and tetanus vaccines. Though this does not provide 100% immunity, by the time the child is 15 months old they should have had enough of the vaccine to fight off a pertussis infection quite well. However babies who have had only the first few doses of the vaccine are still at great risk. Adults and older children should receive a booster shot to prevent the spread of pertussis
New booster vaccines became available in 2005 that offer continued protection against pertussis, diphtheria and tetanus for adolescents and adults. These vaccines have been added to the recommended schedule of vaccinations for adolescents. Adults with routine contact with infants less than 12 months of age should receive a booster dose.
To stem the rising incidence of pertussis, the American Academy of Pediatrics (AAP) is recommending that kids 11-18 years old get a booster shot of the vaccine, ideally when they're 11 or 12 years old.
To reduce the spread of pertussis from unprotected adults to infants, in November the Centers for Disease Control and Prevention (CDC) recommended that adults ages 19 to 64 get a newly-formulated booster shot of tetanus, reduced diphtheria, and acellular pertussis (Tdap vaccine) to replace the previously recommended 10-year tetanus-diphtheria (Td vaccine) booster. Getting the booster shot is especially stressed for adults who will have close contact with an infant who is less than 1 year old, ideally at least 1 month before the contact.
Respiratory etiquette and good hand washing.
Keep infants away from people with coughing illnesses.
KEEP SCROLLING DOWN TO SEE NATALIE CLAIRE'S PICTURES AND STORY:
Natalie Claire's Story (A Fight Against Pertussis)



Natalie was about 6 weeks old when it began. It began with a a runny nose, sneezing, low-grade fever and mild, occasional coughing. Nothing too major. I took her to the doctor just in case, they said it was a cold and not much you could do for it. Slowly, her cough got worse and worse, the other symptoms disappeared, but the cough was stubborn and it continued to get more severe. We took her back to the doctor and they said it was a chest cold, for the next month and a half we took Natalie back and forth to the doctor even different doctors, because she could not get well. Natalie had recently gotten her first vaccinations, they were delayed because she had been sick. The coughing was always the worst at night, but I became very concerned when Natalie began to vomit and turn blue during coughing fits. The coughing would wear her out so much she would become lethargic. But every trip to the doctor was the same scenario: she was just dealing with a bug, a cold, a virus, a cough and she would be fine. No matter how hard I tried to express how scared I was and how NOT normal and severe I thought her cough was, they did not listen. And for some reason, she never seemed to cough in front of the doctors, not even one time. And they did not listen to me, even when I told them there was a funny sound at the end of her coughing fits, sounding like her grasping for air with a "whoop" to it.
Finally on Feb. 23 2009 after several episodes, and exhausting all the resources I had around me, I made the decision that we would take Natalie to the well known Children's hospital (Scottish Rite) E.R. in Atlanta. I knew that Natalie was not doing well and I actually had felt that whatever this was may kill her, that she may die in my arms during a coughing fit. I had never felt so helpless in my life. I was afraid for my husband to leave me alone with her because he knew baby CPR and I did not. My husband was at work the night we decided to go, and I picked him up on the way there, I remember knowing in my heart and in my gut, that we HAD to hurry. I knew somehow, even though I knew nothing about pertussis, I knew our baby was so sick, and desperately needed help. I never felt so relieved as I did when we got there, I knew she was in good hands then.
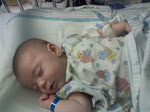
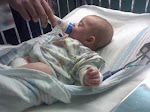
Upon arrival, they said they could tell her oxygen was low by her skin tone and the pattern to her skin. They checked her oxygen level (no one had ever done this at this point) and it was 79, that is deathly low. Immediately they started her on oxygen. It took about 5 minutes of listening to her chest and to what my husband and I were saying for them to say "We think she has pertussis, and she is VERY, VERY sick." They ran a a series of blood tests, nose swabs, mouth swabs, chest x-rays and started pumping 3 different antibiotics, fluids and other antibody medications into her right away. She remained on the oxygen during all of this. Her oxygen would hover around 85 with assistance, except during the coughing fits, in which it would plummet. They admitted my baby girl (she was only 3 months old and tiny for her age) into the PICU right away, they said they did not know if she would make it through the night, NO mother wants to hear that. I watched her struggle to breathe and STOP breathing. I watched her fight a fight her body was not big enough to fight.
By a miracle of God, she did make it through that night and every one after that, but she remained in the hospital for a while. She finally stabilized. She stayed in PICU for a few days and then was moved to the reg. pediatric floor to finish recovery, isolation and medications. They said we had come JUST in the nick of time, one more day and Natalie would have lost her life. She tested positive for pertussis and as a complication of pertussis she also had severe double pneumonia. She left the hospital much better than she was, but she continued to cough for weeks and weeks (they call it the 100 days of coughing). She suffered from lasting effects of the pertussis for a very long time, she still does breathing treatments and sees her pediatric pulmonologist on a regular basis. The pneumonia and pertussis left lots of scar tissue in her tiny lungs, but today she is doing very well. That was almost a year ago. The doctor said it a million times, we are so lucky to still have her, it was a true miracle. We do not know how Natalie got pertussis. I had a bad case of bronchitis soon after having her, also her older brother had a birthday party around this time with many small kids and adults in our house. One way or another someone had it and never even knew it and she got it and we almost lost her forever. I think it came from me, at the time I was not vaccinated with the booster shot of pertussis because I did not know to do so, and I had been very sick. I never knew I could give her something that would kill her. I even remained out of her face and away from her (with the help of my husband) until I got better.
Many infants who contract pertussis do not have that same fate. It takes many infant's lives. Their bodies simply are not big enough to fight it. Adults, children, and infants alike can get pertussis, but small children, especially infants, are the ones it seems to affect the greatest and with the most severe cases. No one should have to watch their child fight for their life when it can be prevented and THIS is why I write this blog, for my daughter, and every other child and family affected by this disease. Adults do not know they have pertussis. It comes out as a cold or even milder in them and they rarely get diagnosed with it. The diagnosis at worst with adults is usually bronchitis and they get over it, never knowing they could have possibly had pertussis and it could be fatal for an infant that they love.
Also in memory of Lane Grady who recently lost his life to pertussis at 5 months old and all the other babies who have lost their life to this disease. Had I known to get vaccinated, my daughter would probably have never gotten this.